Blood Test Breakthrough: New Biomarker Could Revolutionize Alzheimer’s Diagnosis
Could a simple blood test be the key to unlocking earlier adn more accurate Alzheimer’s diagnoses? A groundbreaking study is suggesting exactly that, offering hope for millions of Americans affected by this devastating disease and related dementias.
Researchers have identified a blood-based biomarker, P-TAU217
, that shows remarkable accuracy in distinguishing Alzheimer’s disease from other forms of dementia, including frontotemporal lobe dementia (FTLD). This is a significant leap forward, as current diagnostic methods like PET scans and cerebrospinal fluid tests are often expensive, invasive, and not readily accessible to everyone.
Think of it like this: for years, doctors have relied on complex and sometimes risky procedures to diagnose Alzheimer’s, similar to how football coaches used to rely solely on game film to scout opponents. Now, this blood test could be like having access to advanced analytics – a quicker, easier, and more precise way to understand what’s happening.
The study, published in JAMA Neurology, analyzed blood samples from a cohort of 349 individuals, meticulously correlating blood biomarker levels with post-mortem brain pathology. This rigorous approach strengthens the findings and adds considerable weight to the biomarker’s potential.
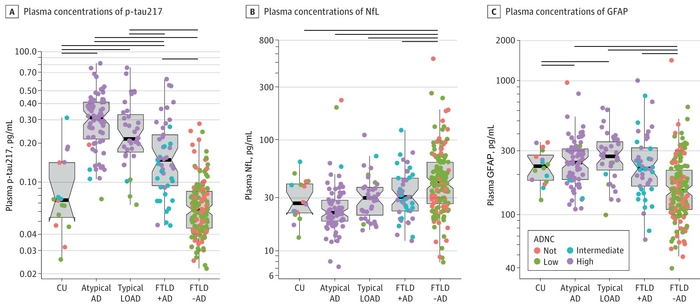
The research team, a collaboration between Yonsei University, Gangnam Severance Hospital, and the University of California, San Francisco (UCSF), didn’t just look at P-TAU217 in isolation.They also analyzed other biomarkers like NFL (a marker of neurological damage) and GFAP (an indicator of nervous system inflammation).The results were compelling: P-TAU217 demonstrated significantly higher diagnostic accuracy (AUC of 0.95) compared to NFL (AUC of 0.73) and GFAP (AUC of 0.75). In simpler terms, P-TAU217 was the clear MVP in identifying Alzheimer’s pathology.
It is indeed significant in that the world’s first to accurately detect Alzheimer’s pathology in various dementia patients,
said Professor Cho Han-na, a lead researcher on the study.
One crucial finding was that approximately 23% of patients initially diagnosed with FTLD also exhibited Alzheimer’s pathology. These individuals with mixed dementia showed worse performance on cognitive tests and more severe brain atrophy, highlighting the importance of accurate diagnosis for tailored treatment strategies. This is akin to a baseball manager understanding a player’s strengths and weaknesses to optimize their performance – accurate diagnosis allows for more effective intervention.
Though, its significant to acknowledge potential counterarguments. Some might argue that relying solely on a blood test could lead to misdiagnosis,especially in complex cases. While P-TAU217 shows high accuracy, it’s unlikely to be a perfect solution. Further research is needed to determine the optimal way to integrate this biomarker into clinical practice, potentially in conjunction with other diagnostic tools.
Despite these considerations, the potential benefits of a readily available and accurate blood test for Alzheimer’s are enormous.Early and accurate diagnosis can empower patients and families to make informed decisions about treatment, care planning, and participation in clinical trials. It could also accelerate the advancement of new therapies by allowing researchers to identify and enroll appropriate participants more efficiently.
Areas for Further Examination:
- Longitudinal Studies: How does P-TAU217 change over time in individuals at risk for Alzheimer’s?
- Diversity in Study Populations: Does the accuracy of P-TAU217 vary across different racial and ethnic groups?
- Clinical Implementation: What is the most effective way to integrate P-TAU217 testing into routine clinical practice?
this research represents a significant step forward in the fight against Alzheimer’s disease. While more work remains, the promise of a simple blood test to revolutionize diagnosis offers a beacon of hope for the future.
Key Findings: P-TAU217 vs. Othre Biomarkers
To better illustrate the impact of P-TAU217,here’s a comparative analysis of its performance alongside other biomarkers:
| Biomarker | Diagnostic Accuracy (AUC) | Primary Functionality | Key Advantage | Limitations |
|---|---|---|---|---|
| P-TAU217 | 0.95 | Detects phosphorylated tau protein associated with Alzheimer’s pathology | Highest diagnostic accuracy; sensitive to early-stage changes; easy to administer via blood draw | Requires further validation; potential for rare false positives; Not a standalone diagnostic tool |
| NFL (neurofilament Light Chain) | 0.73 | Indicates general neurological damage | Useful for detecting overall neurodegeneration | Lower specificity; Doesn’t distinguish between Alzheimer’s and other dementia types; Damage not unique to Alzheimer’s |
| GFAP (Glial Fibrillary Acidic Protein) | 0.75 | Measures nervous system inflammation | Provides insight into inflammatory processes | Less specific for Alzheimer’s; May be elevated due to other neurological conditions |
| PET Scans (Amyloid/Tau) | High (dependent on scan type) | Visualizes amyloid plaques and tau tangles in the brain | Highly accurate; Allows for direct visualization of key pathologies | Expensive; Invasive; Limited accessibility; Requires specialized expertise |
| Cerebrospinal Fluid (CSF) Analysis | High (dependent on analysis) | Measures levels of amyloid, tau, and other proteins | Accurate; Reflects brain pathology | Invasive; Requires lumbar puncture; Risk of complications |
FAQ: Your Questions Answered About the Alzheimer’s Blood Test Breakthrough
This section addresses frequently asked questions about the new Alzheimer’s blood test, providing clear and concise answers to help you understand the implications of this research.
What exactly is P-TAU217, and why is it crucial?
P-TAU217 is a specific form of the tau protein, a key protein involved in Alzheimer’s disease. The “P” stands for phosphorylated, meaning a phosphate group has been added to the tau protein.In Alzheimer’s, tau accumulates abnormally within brain cells, forming tangles. P-TAU217, measured through a simple blood test, can indicate the presence and severity of these tangles, offering an early and more accessible way to detect the disease.
How accurate is the P-TAU217 blood test?
The study showed that P-TAU217 has a high diagnostic accuracy, with an AUC (Area Under the Curve) of 0.95. This indicates a strong ability to differentiate between Alzheimer’s disease and other forms of dementia.Specifically, it is more accurate than existing blood-based markers. However,while promising,no diagnostic test is perfect; further research is needed to refine its use in clinical settings.
What are the advantages of this blood test compared to current diagnostic methods?
Compared to current methods like PET scans and cerebrospinal fluid (CSF) analysis, the blood test offers notable advantages: it is indeed less invasive, more accessible (as it can be done in most clinics), and more affordable. PET scans and CSF analysis can be expensive, require specialized facilities, and have potential risks.This blood test provides a faster and easier screening method.
Will this blood test replace all other diagnostic tools for Alzheimer’s?
Not necessarily. While highly promising, the P-TAU217 blood test is unlikely to entirely replace other diagnostic tools. It’s more likely to be used in conjunction with them. Such as, it could initially be used as a screening tool to identify individuals who may need further, more in-depth testing, such as MRI or PET scans.
When will this blood test be available to the public?
The timeline for widespread availability is currently uncertain.Further studies are needed to validate the test across diverse populations and to establish its optimal use in clinical practice. Regulatory approvals from bodies like the FDA would also be required. Though, considering the promising results, the anticipation is high. Stay tuned for updates as research progresses.
How can this blood test help in the development of new Alzheimer’s treatments?
early and accurate diagnosis is critical for advancing treatment development. The blood test can help identify individuals who are eligible for clinical trials earlier in the disease process. In studies, this will permit researchers to more efficiently enroll participants. The test also allows scientists to monitor the effectiveness or potential impact of new drugs. This acceleration could substantially speed up the process of bringing new therapies to patients.
Are there any potential risks or drawbacks to using this blood test?
While the blood test is a promising tool, like any medical test, it has potential drawbacks. There’s a possibility of false positives or false negatives, which can impact a patient’s treatment journey. Further research is therefore required to hone diagnostic performance and interpret results accurately in various contexts, with various other contributing factors such as related illnesses and medications.
Where can I find more information about Alzheimer’s disease and this research?
Reliable sources of information about Alzheimer’s disease include the Alzheimer’s Association, the National Institute on Aging (NIA), and the World Health Organization (WHO). For details on this specific research, you can consult the original study published in JAMA Neurology.
Disclaimer: This article is intended for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.